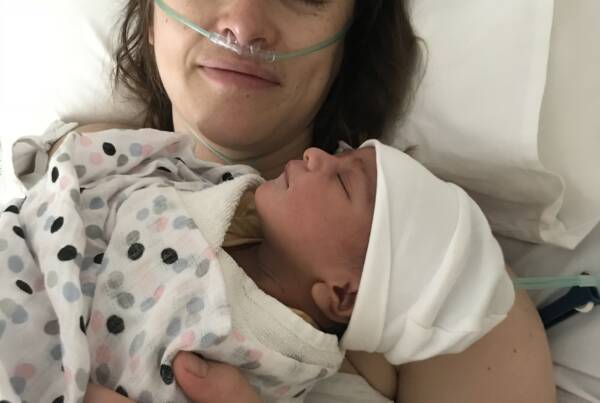
Writing by Claire Wastell // Photograph by Sol Avena // The stigma that comes with the term anorexia had held back my recovery for years. I didn’t want people to talk about me and think of all the loaded connotations that come with the label anorexia.
Writing by Claire Wastell // Photograph by Sol Avena
I suffer from a mental illness. So many of us do, but we don’t talk about it. We don’t feel comfortable going on a coffee date with a friend, and speaking about our anxiety, depression, or fears. We think so much about what that friend will now think of us. Will they presume we are unstable, easily disturbed, highly on edge, or prone to panic attacks? And will this influence how this person treats you—perhaps they will be more careful or sensitive, or, at worst, think you are too difficult to deal with, and no longer want to associate with you?
We don’t talk about mental illness because we often struggle to associate our experience with the symptoms the media tells us are a sign of these issues. This creates a stigma, and we become worried what others will think when they find out about our illness. So we stay silent and don’t talk about the issues we have been dealing with. We simply smile. But is this really helpful? How can we go about dealing with our issues when we feel we can’t even identify them, let alone talk about them? In this article I explore these ideas within my own struggles and explore how the first way to decode mental illness is to acknowledge the stigma and stereotypes. To be able to admit that they may not be what we personally are experiencing, but never the less, does not mean that we do not have a mental illness. We do need to find help, support, and seek forgiveness of ourselves.
I think we are all a little bit scared to identify with a mental illness, because of the stereotypes associated with this label. I know this prohibited my recovery and working towards dealing with my problems because I didn’t want to identify with the illness I was experiencing. It is true though that the issues I was having towards my mental illness were NOT the problems society told me I should be having. In 2015, I was diagnosed with anorexia nervosa, something I refused to admit I had. Never had I starved myself. I didn’t have body image issues, and never desired to be thinner. When people talked about my condition calling it an ‘eating disorder’, I refused to acknowledge it. I would get so frustrated when people assumed the reason I was walking my dog, or not wanting butter on my sandwich, was because of the anorexic ‘thoughts’ which were taking over my thinking, when really, I found walking my dog a huge stress relief, and I have never had butter on my sandwiches in my life.
I was admitted three times into the Children’s Ward between 2015-2016 for two week periods due to a low heart rate and blood pressure drop, as well as not having natural periods due to low body weight. These were the facts, and according to the diagnosis in the DSM for an eating disorder, I fitted the criteria. I had lost weight and maintained an unhealthily low weight, I was experiencing physiological body changes due to this weight loss, and it was assumed that this was also affecting my thinking. My first admission was traumatic, my doctor was worried about my heart, and had sent me to the hospital which terrified both my mother and I. I didn’t even know that hospitals took on this kind of problem, and next thing I knew, little 16 year old me was forced to being confined to bed in a shared room with screaming babies and girls with severe eating issues. I was taken everywhere in a wheelchair, and even being watched in the shower! I was angry because I was treated like I had anorexia, and was asked about my fear of foods and distress around eating, when really none of this affected me. I loved food, and suddenly I was asked to track calories to ensure I was being feed enough to gain weight.
It was the fact I couldn’t relate to the illness I was experiencing which led to a downward spiral that ended with me losing around 10 kilos following my last admission in the Children’s ward, and moving states to go to college. Before leaving I would not acknowledge I had a problem. I thought that eating disorders were all body image, wanting to get skinny, and hating myself, when really I felt great, would never miss a meal, and loved to go walking and dining with friends. I couldn’t understand why people said I had anorexia, when I didn’t relate to any of the so-called symptoms.
Living alone came with a variety of new challenges, but none more so than realising I actually couldn’t feed myself properly. I ate regularly and consistently, but because I refused to recognise I had problems with food, I quickly lost weight because I simply wasn’t eating enough of the food my body needed. I started to experience this strange sensation where my body began to drop more and more weight, while my mind seemed to exist entirely separate to it. My mind wanted to take every opportunity and DO everything, but my body began to look like a skeleton. I was so lost. I wanted to travel, to go out with friends, to run, to work—but my body lacked the energy and strength. My mood dropped and I was a mess. I couldn’t stop the weight from dropping off. On returning home, my Mum could no longer look at me, it was too distressing, and I was admitted as an inpatient in a psychiatric ward in order to regain some of the weight I had lost. I was now at a weight I had not been since I was 11 years old, and I was scared.
Yet I still found I couldn’t relate to the anorexia that society advertised. I did some reading while I was in hospital and found Carrie Arnolds’ Decoding Anorexia, a book which discusses the biological symptoms of developing anorexia, including its strong genetic connection, and ways the brain does not process things the way others do. It speaks of both the biological and environmental factors that can lead to eating disorders, and how you can have an eating disorder without exposure to the media, models, and expectations of body image. Studies show that places such as Ghana and China have equal rates of anorexia, and cases have been reported amongst groups such as the Amish who are never exposed to such media platforms. It has been found that 86% of your chance of developing anorexia is genetic, which made sense to me as my mother, grandmother, and other members of my family have experienced various types of eating problems. In fact, the brain functions involved in perception and anxiety—called the insula—do not actually function as well in people who develop anorexia. These discoveries, in addition to the knowledge of my fast metabolism, made me finally accept and acknowledge I have an eating disorder—just not the one society suggests.
This was the first step towards my recovery, because I realised I had a problem that needed FIXING for the first time. I became ready to start my recovery and heal myself. The stigma that comes with the term anorexia had held back my recovery for years. I didn’t want people to talk about me and think of all the loaded connotations that come with the label anorexia. Something that is meant to help and identify my issues actually became pivotal in my sickness. When talking to others with a range of mental illnesses, I soon found the same issues. A friend with depression confided in me that she only came to terms that she had depression when it reached a tipping point in her life and she could no longer cope. Before that, she had been unable to identify this as depression, as she didn’t have suicidal thoughts or constant low moods, and wasn’t socially isolated: all symptoms commonly associated with the illness. My friend soon realised that what she had been feeling was depression, just not the kind that depression is normally labelled as. This made me realise the importance of decoding the biological side to mental illness, and removing the stigma of these problems. To talk about how we are feeling, and realising that each person is DIFFERENT with unique problems. Yes I have anorexia, but I don’t have the severe related body weight issues. The first step to my recovery was feeling like I could admit that. And this is the way, I think, we are going to tackle mental illness.